Everything is connected. Our health and the health of our planet.
With global temperatures continuing to rise, we need to adapt to the effects of climate change even as we urgently tackle its causes.
This means protecting the health of everyone — here in British Columbia, across Canada, and around the world — so together we have the strength and resilience to make the world a better place, today and for future generations.
To succeed, we need healthcare systems that are adaptable, equitable, and environmentally sustainable — planetary healthcare systems.
The UBC Faculty of Medicine is helping to future-proof healthcare systems — and our health and the health of our communities — through research, innovation, education, and partnerships.
Here’s how.
Julie Jacques, Elder, Takla First Nation; Dr. John Pawlovich, Rural Doctors’ UBC Chair in Rural Health; and Dr. Sean Ebert, Clinical Instructor, Department of Family Practice
Urban planning for healthier childhood development
Air pollution puts children at increased risk for ADHD and other neurodevelopmental issues. Dr. Matilda van den Bosch is uncovering the protective effects of urban greenspaces.


Improving respiratory health through food
Respiratory illnesses are among the leading causes of hospitalization and premature death in Canada. Dr. Emily Brigham is investigating how certain foods can protect and improve our respiratory health.
A prescription for better mental health
Research shows that spending time in nature benefits our mental and physical health. Dr. Melissa Lem’s award-winning initiative, created in partnership with the B.C. Parks Foundation, enables healthcare providers to ‘prescribe’ time in nature to their patients — in the form of activity plans and free passes to national parks and other outdoor spaces.


Healthy aging from society to cell
Many different factors affect how we age, from our genes to our social lives to our exposure to climate hazards such as wildfires. Dr. Michael Kobor and the Edwin S.H. Leong Centre for Healthy Aging are unlocking the secrets to living longer, healthier lives in a changing environment.
Genomics for more effective public health policy
Dr. Chris Carlsten and researchers from the Air Pollution Exposure Laboratory have identified genetic variants that make some people more susceptible to air pollution-related health complications. Their findings have the potential to transform the way we treat and prevent respiratory illnesses at the population level.

Dr. Kathleen Martin Ginis, Director, Centre for Chronic Disease Prevention and Management and Reichwald Family UBC Southern Medical Program Chair in Preventive Medicine
The Pathways to Equitable Healthy Cities initiative
The design of our cities influences our health — and the health impacts of climate change. Dr. Michael Brauer leads a multidisciplinary team of Vancouver researchers that is finding innovative ways to reduce health inequality through urban planning, design and policy to create healthier communities for everyone.


Improving respiratory health services for Indigenous communities
Respiratory illnesses affect Indigenous peoples more than any other group in British Columbia. Dr. Brittany Bingham is working with elders and community members to make respiratory health services more accessible, more responsive and culturally safer for patients.
Building resilient and accessible health networks in a changing climate
UBC’s distributed medical education program trains doctors and health professionals in rural, remote and urban communities across B.C. — building networks of health professionals in every corner of the province. This increases the reach and resiliency of the healthcare system while also helping to ensure equitable, high-quality care even during periods of climate disruption.

Virtual care for rural and remote communities
The brainchild of UBC’s Dr. John Pawlovich, Dr. Ray Markham, and Dr. Kendall Ho, the peer-to-peer Real-Time Virtual Support (RTVS) pathways connect physicians and health professionals in rural, remote and First Nations communities with collegial support from emergency medicine to hematology to dermatology. This makes it easier for patients to receive timely and appropriate care without always needing to travel to a major urban centre — or worry that climate hazards will disrupt their treatment.
Drone-based emergency medical supply delivery
In East Africa and northern British Columbia, PhD candidate Marie Paul Nisingizwe and Dr. John Pawlovich are helping to bring lifesaving medical supplies to remote and rural communities faster than ever before using drone technology.


A million vaccine doses in a single test tube
Climate change has the potential to increase the frequency and severity of pandemics. Dr. Anna Blakney is developing self-amplifying RNA technology that is 100 times more efficient than the mRNA used in current vaccines, and equally safe. It has the potential to make population-level immunization faster, more equitable, and more cost-efficient.
Emergency preparedness for Indigenous and remote communities
In partnership with Carrier Sekani Family Services (CSFS), and the 10 First Nations served by CSFS, PhD candidate Justin Turner and Dr. Pat Camp are studying the health impact of recent wildfires on Indigenous communities in northern B.C. — with the goal of supporting the Nations as they develop their emergency health response practices.


Effective public health messaging systems
When climate hazards happen, we all need timely, relevant advice and information to protect ourselves and our communities. Dr. Sarah Henderson is leading the design of emergency public health messaging systems for extreme heat and wildfire events in B.C.
Better care in disasters for children with special healthcare needs
Climate disruption puts children who need regular and uninterrupted medical care at particular risk. In a rapid scoping review, Drs. Craig Mitton and Esther Lee show how careful planning and communication between healthcare providers and the families of children with special health care needs is needed to safeguard their care and treatment.

Planetary Healthcare Lab
The only academic entity of its kind in the world, UBC and Vancouver Coastal Health’s Planetary Healthcare Lab brings together experts and thought leaders from a wide range of disciplines to reimagine health systems that can be better for both the patient and the environment. With support from UBC’s Strategic Investment Fund, they are tackling everything from medical supply chain emissions, to unnecessary patient testing and treatment, to hospital food-related pollution.

More sustainable laboratories, classrooms and offices
In line with UBC’s 20-Year Sustainability Strategy, the Faculty of Medicine is taking action to reduce the environmental impact of labs, classrooms and offices through initiatives like medical glove and mask recycling, remote learning, and more.
Lower-emission radiology
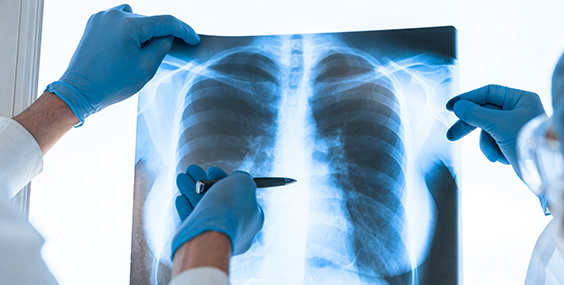
Medical imaging technology — from simple X-rays to high-resolution MRI — is an essential but emission-intensive tool for medical professionals. Dr. Maura Brown is developing greener radiology protocols that will help radiologists reduce their carbon footprint without sacrificing diagnostic precision.

Toward greener, healthier hospital menus
Food waste and malnutrition cost Canada billions each year. Dr. Annie Lalande is working with health partners to transform hospital food systems, serving up meals that are good for our bodies and the planet.
New proposed professional degree to tackle the global health impacts of climate change
The School of Population and Public Health is in the early stages of developing a new graduate-level professional degree program specifically focused on climate change and other systemic forces that impact health on a global scale. The goal of the program is to equip learners with the knowledge and skills to tackle the poor health outcomes and inequities created by these forces.


Climate change adaptation through occupational science
Occupational therapy and occupational science can play a vital role in helping people with disabilities to adapt and thrive when affected by climate hazards. Dr. Ben Mortenson is working to develop lectures, tutorials and workshops on climate change adaptation and mitigation for Master of Occupational Science students.
Planetary health for doctors-in-training
With support from UBC Sustainability, Dr. Adrian Yee is leading the development of new, planetary health-focused curricula for UBC’s Doctor of Medicine (MD) program. The goal is to train learners in the latest knowledge and practices and empower them “to challenge the status quo and envision what it means to thrive as people on this planet.”


Greener family medical practice
A team of UBC family practice resident doctors have created a special training module to help physicians reduce their carbon footprint and become planetary health advocates. Geared toward both resident and practicing doctors, the training module offers practical advice on reducing medical practice emissions and encouraging patients to make healthy, planet-friendly lifestyle choices.
Never miss an issue of Pathways
Pathways — the UBC Faculty of Medicine’s digital magazine — features stories about cutting-edge health education, breakthrough research, and biomedical innovations that are making a difference in British Columbia and around the world. Discover the impact of our people and programs.